Anticoagulation Management
Anticoagulants are medications that help prevent existing blood clots from growing larger and the formation of new blood clots by increasing the amount of time it takes a blood clot to form. Anticoagulants help to prevent unwanted clotting by increasing the amount of time it takes blood to clot. Warfarin, is one type of anticoagulant and our Warfarin therapy program is further discussed below.
There are a number of reasons as to why anticoagulant therapy may be indicated:
- Deep Vein Thrombosis: This term refers to a blood clot that forms in one of the large veins in the leg or arm. These clots cause damage by blocking blood flow, which leads to swelling and discomfort in the extremity.
- Pulmonary Embolus: A blood clot, that forms in or travels to the lungs is called a pulmonary embolus. These clots are dangerous because they result in lack of oxygen. Shortness of breath and chest pain are symptoms of an embolus in the lung. The severity of the problem depends on how big the clot is and where it lodges in the circulation.
- Atrial Fibrillation: This condition causes an abnormal rhythm and rate of the heart. As a result, blood cannot be pumped out of the heart as efficiently as it should be. This can cause the blood to become sluggish and possibly clot. If a clot breaks off, it can travel through the circulation, where it might lodge in a vessel and cause serious damage such as a stroke or heart attack.
- Artificial Heart Valve: Because an artificial heart valve is made of a synthetic substance, the body does not recognize it and attempts to protect itself against it. Clots may form as a result.
- Hereditary Disorders: There are certain proteins formed by the body that either cause blood to clot or prevent it from clotting. Protein C and S and antithrombin III help to prevent clots. Some people are born with a deficiency of these proteins and are at risk for blood clots. Other substances, such as anticardiolipin antibodies, when present, can cause clotting. Some people develop these antibodies and become prone to blood clotting.
Length of time on Warfarin
Length of time on anticoagulation therapy varies from patient to patient. For patients with a single episode of deep vein thrombosis or pulmonary embolus, treatment is between three and six months. In most cases, people with atrial fibrillation will need to take Warfarin for the rest of their lives, as will patients with recurrent blood clots, hereditary disorders, and artificial heart valves. Of course, treatment is individualized for everyone, and you will be an important part of the decision-making process.
Normal Blood Clotting
When an injury occurs that causes bleeding, a blood clot will form to stop the bleeding and protect against infection. When the injured blood vessel has healed itself, the clot is no longer needed and is gradually reabsorbed by the body. Substances in the blood, called clotting factors, work to ensure that the blood flows smoothly and that it does not become too thick or too thin. Under normal circumstances, these processes work quite well.
Under certain circumstances, the body becomes more prone to developing blood clots abnormally. This can lead to blood clots in areas that cause harm, such as in the heart, lungs, brain, or extremities. If a clot forms in such an area, it might cause a blockage in the circulation and hinder blood flow. More seriously, a piece of the clot might break off and travel through the circulation. This can be a potentially life-threatening event. Certain clotting abnormalities are inherited. Some people develop clots in response to specific triggers, such as prolonged immobility that causes sluggish blood flow. This can happen during prolonged surgical procedures or if an extremity is immobilized in a cast. It can also occur in patients who are immobile because of paralysis. Finally, pregnancy is a time when the body is more prone to blood clotting. This is a protective mechanism that occurs near the end or pregnancy, as the body is preparing for delivery, to prevent excessive blood loss.
In most cases, abnormal clotting does not usually occur, but certain conditions do make it more likely. Your doctor may opt to treat you with a “blood-thinning” medication to prevent you from developing a blood clot, or you may already have a blood clot and are being treated with “blood-thinners” to prevent it from getting worse or traveling to other parts of your body.
Warfarin: How it Works
Natural proteins that are present in the blood help the blood to clot when you are injured. Some of these proteins are made with the help of Vitamin K. Warfarin interferes with the function of vitamin K, which decreases the amount of clotting proteins formed in the body. Therefore, Warfarin increases that time that the body normally takes to form clots. This protects the body from forming harmful clots. Warfarin is commonly known as a blood-thinner. This is not really a correct term because the blood does not actually become thinner; it simply takes a longer time to form a clot.
Monitoring Warfarin Therapy
It is important to monitor very closely the effect of Warfarin on the blood. This medicine is not like most others, where you take the same amount each day. Many things can interfere with or enhance the effects of Warfarin. For that reason, your blood will be checked very frequently at the start of your treatment with this medication. Once you are stable, it will be checked approximately once a month. If your condition changes, you start a new medication, or if you become ill, we might temporarily need to check your blood more frequently again.
The blood test performed is called a prothrombin time; also known as a Protime test or PT/INR. This test can be performed by sending a blood sample to the laboratory, or it can be performed at our office by a fingerstick. The fingerstick gives us an immediate result which is convenient for monitoring your Warfarin dosage. Three numbers are obtained from your blood sample:
- Prothrombin time (measured in seconds)
- Prothrombin time ratio
- Protime International Normalized Ration (INR)
These numbers are used to determine if you are taking the correct amount of Warfarin. In a normal person who is not on Warfarin, the protime will be between 11-13 seconds, the ratio will be 1, and the INR will be less than 1. The number used to determine your Warfarin dosage is the INR. For patients on anticoagulation therapy, the INR is kept at a number ranging anywhere from 1.5 to 4.0. If the number is too low, your medication dosage will be increased. If it is too high, your dosage will be decreased. The INR range established for you will depend on your particular condition and lifestyle needs.
Side Effects of Warfarin
The reason why your blood is checked so frequently is because side effects of Warfarin can be dangerous. If too much Warfarin is being give, bleeding can result. It might be very minor, such as gum bleeding while you brush your teeth; but more serious episodes of bleeding might occur, such as bleeding from the stomach or into your brain.
Results of Too much Warfarin: Bleeding
- Gum bleeding while brushing teeth
- Occasional nosebleed
- Easy bruising
- Prolonged bleeding after minor cuts
- Prolonged menstrual bleeding
You might notice any of the above symptoms from time to time. If you are unsure whether bleeding is significant and represents a problem, it is best to call the clinic and report it. It may be necessary to decrease your dose or have your protime checked to be sure.
Major Bleeding
- Blood in urine or stool
- Black, tarry stools
- Coughing up blood
- Severe headache
- Severe bleeding into whites of eyes
- Any bleeding that continues or is of excessive amount
Result of Too Little Warfarin: Blood Clotting
Call your doctor immediately if you notice any of the following signs and symptoms of a blood clot:
- Sudden weakness in any limb
- Numbness or tingling anywhere
- Visual changes or loss of sight in either eye
- Sudden onset of slurred speech or inability to speak
- Dizziness or fainting
- Severe pain or swelling in an extremity
- Shortness of breath or chest pain
All of these signs and symptoms can be serious. Remember: Call your doctor immediately if any of them occur.
Things That Interfere with Warfarin
Many medications and things that you might eat or drink can either increase or decrease the effects of Warfarin.
Vitamin K and Alcohol
Because vitamin K counteracts with Warfarin, you might not be getting enough Warfarin if you suddenly begin eating increased amounts of foods high in vitamin K.
Also, drinking alcohol can affect the amount of Warfarin in your blood. Alcohol can either increase or decrease the effect of Warfarin. It is not always predictable.
The most important point to remember is to be consistent in what you eat and drink. Having a spinach salad is not harmful if you don’t suddenly decide to eat a whole truckful at one sitting. The same goes for alcohol. The key is to remember moderation. What is harmful is bingeing on things that interact with Warfarin.
Other Medications
This is a very important area for you to remember. Many medications act either to increase or to decrease the effects of Warfarin. Probably the most common medications to avoid are products containing aspirin. This is because Aspirin also acts to decrease blood clotting, so it would be dangerous to be taking two medications that affect blood clotting. Also, non-steroidal medications are not to be taken while on Warfarin.
Over-the-Counter (OTC) Drugs
Following is only a partial list of the over-the-counter products that you should not take while on Warfarin. There are others. You must read labels and ask questions before taking any medication to ensure that it does not contain any harmful substances.
DO NOT TAKE THESE OVER-THE-COUNTER MEDICATIONS:
- Advil
- Aleve
- Alka-Seltzer
- Ascriptin
- Aspirin
- Bayer
- Bufferin
- Ecotrin
- Empirin
- Ibuprofen
- Medipren
- Motrin
- Naprosyn
- Nyquil
If you need to take medication for pain or a cold, it is best to ask your doctor or pharmacist for suggestions. The following products, however, are safe to take.
YOU MAY TAKE THESE MEDICATIONS SAFELY:
- Acetaminophen
- Allerest
- Anacin-3
- Benylin & Benylin-DM
- Chlor-Trimeton
- Contac
- Drixoril
- Maalox
- Mylanta
- Robitussin and Robitussin-DM
- Sudafed and Sudafed-Plus
- Tylenol
Note: If you use antacids, such as Maalox or Mylanta, for heartburn, take them at least two hours before, or two hours after your Warfarin.
Prescription Drugs
Many prescription drugs interfere with Warfarin. Tell all of your doctors that you are taking Warfarin, so they will know which medications can be prescribed for you. It is also a good idea to have all of your medications filled at the same pharmacy, so that your pharmacist will be alert to any medications that you should not be taking with Warfarin.
Herbal Products
Caution should be exercised when herbal products are taken together with Warfarin. The use of herbal products may increase or decrease the effects of Warfarin. Specific botanicals reported to affect Warfarin therapy include the following: bromelains, danshen, dong quai garlic, ginger, ginkgo biloba, green tea and ginseng are associated most often with an increase in the effects of Warfarin. Coenzyme Q10 and St. John’s wort are associated most often with a decrease in the effects of Warfarin.
Warfarin Preparations
Warfarin tablets come in several strengths: 1mg, 2mg, 2.5mg, 4mg, 5mg, 7.5mg, and 10mg. We will try to keep your daily dose the same, but it is possible that you might take different doses on different days. This will depend on your blood results. Most likely, you will have one or two different strengths from which we can combine to make the correct daily dose. Please call if there are any questions regarding your dose.
It is helpful in the beginning to write down your daily dose for the week because you are not familiar with the medication. Also, this is when the medication is most likely to fluctuate in dose. It is also helpful to count out your pills for the week and keep them separated in a pillbox.
Other Health Care Providers (Specialists)
Tell all of your doctors that you are taking Warfarin, so they will know which medications can be prescribed for you. It is also a good idea to have all of your medications filled at the same pharmacy, so that your pharmacist will be alert to any medications that you should not be taking with Warfarin.
Pregnancy
Warfarin cannot be taken by pregnant women. If you are, or are planning to become pregnant, please notify the clinic. For women who must be anticoagulated during pregnancy, there are other safe options available. Warfarin causes birth defects to the developing fetus.
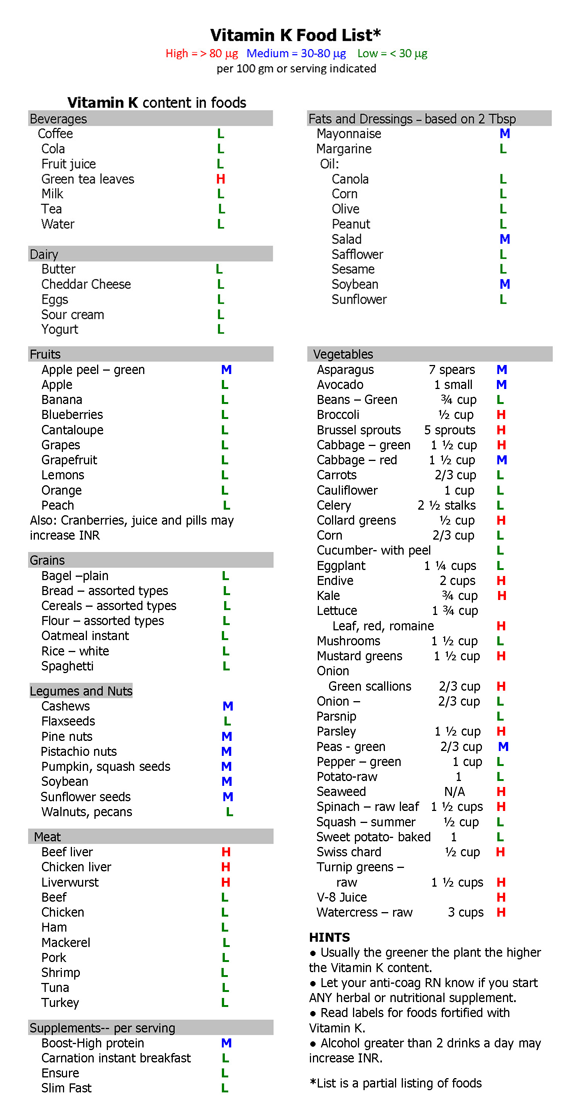
Diet
Below is a list of the Vitamin K content in common types of foods. This is not meant to be an all-inclusive list. If you have any questions, please call the clinic and ask.